- Weight Loss
-
by Skippack Pharmacy
A Common Journey
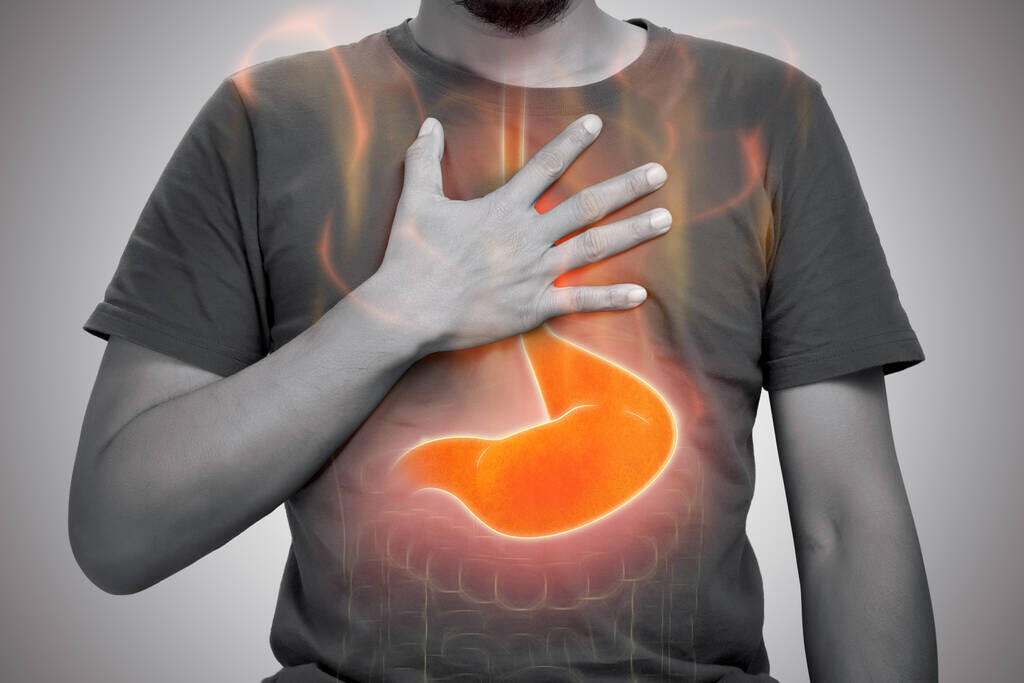
One patient was thrilled when their doctor prescribed a GLP-1 medication to help manage type 2 diabetes and support weight loss goals. The first few weeks went smoothly, but after the second dose increase, something new started—a burning sensation in the chest that seemed to worsen after meals. At first, it seemed like just stress, but the discomfort became more frequent, especially when lying down at night.
The heartburn was affecting sleep and making mealtimes dreaded. There was concern about having to stop the medication that was finally helping reach health goals. But after talking with the healthcare team and making some simple lifestyle changes, the patient learned how to manage the reflux symptoms effectively. Within two weeks, sleep improved and meals became enjoyable again—all while continuing GLP-1 therapy. Here’s what made the difference.
Why GLP-1 Medications Can Cause Heartburn
GLP-1 medications work partly by slowing down how quickly food moves from your stomach into your intestines. This delayed gastric emptying helps you feel fuller longer and supports weight loss, but it can also increase the likelihood of stomach acid flowing back into your esophagus—the tube connecting your mouth to your stomach.
When this happens, you might experience:
- Burning sensation in your chest (heartburn)
- Sour or bitter taste in your mouth
- Feeling of food coming back up
- Discomfort in your upper abdomen
- Bloating or feeling overly full after small meals
- Burping or belching
The good news is that these symptoms are usually manageable with the right strategies, and they often improve as your body adjusts to the medication.
Eating Habits That Help
Eat Smaller, More Frequent Meals
Large meals put extra pressure on your stomach and increase the likelihood of acid reflux. Instead of three big meals, try eating five to six smaller meals throughout the day. Think of it as grazing rather than feasting—your stomach will thank you.
Slow Down and Chew Thoroughly
Eating too quickly can worsen reflux symptoms. Take your time with each meal, put your fork down between bites, and chew your food well. This not only helps with digestion but also gives your brain time to register fullness.
Don’t Lie Down After Eating
This is one of the most important rules for managing reflux. Wait at least 2-3 hours after eating before lying down or going to bed. Gravity helps keep stomach acid where it belongs—in your stomach. If you need to rest, try sitting in a comfortable chair instead.
Elevate Your Head While Sleeping
If nighttime heartburn is a problem, raise the head of your bed by 6-8 inches using bed risers or a wedge pillow. Simply stacking regular pillows doesn’t work as well because it can cause you to bend at the waist, which actually increases pressure on your stomach.
Foods to Avoid
Certain foods are more likely to trigger or worsen heartburn:
High-Fat Foods
Fatty foods slow gastric emptying even more, which can significantly worsen reflux symptoms.
- Fried foods (french fries, fried chicken, donuts)
- Fatty cuts of meat
- Full-fat dairy products
- Creamy sauces and gravies
- Fast food burgers and pizza
Acidic Foods
These can irritate an already sensitive esophagus:
- Citrus fruits and juices (oranges, grapefruits, lemons)
- Tomatoes and tomato-based products (pasta sauce, ketchup)
- Vinegar-based dressings
Spicy Foods
Hot peppers, hot sauces, and heavily spiced dishes can trigger heartburn in many people.
Trigger Beverages
- Coffee (both regular and decaffeinated)
- Alcohol
- Carbonated beverages (soda, sparkling water)
- Mint tea (surprisingly, mint can relax the valve between your stomach and esophagus)
Other Common Triggers
- Chocolate
- Onions and garlic (especially raw)
- Peppermint
Foods That Are Easier on Your Stomach
Focus on foods that are less likely to trigger reflux:
Lean Proteins
- Skinless chicken breast
- Turkey
- Fish (baked or grilled, not fried)
- Egg whites
Whole Grains
- Oatmeal
- Brown rice
- Whole grain bread
- Quinoa
Vegetables (non-acidic)
- Leafy greens
- Broccoli
- Cauliflower
- Cucumbers
- Green beans
- Potatoes (baked or boiled, not fried)
Fruits (non-citrus)
- Bananas
- Melons
- Apples
- Pears
Healthy Fats in Moderation
- Avocado (small amounts)
- Olive oil (used sparingly)
- Nuts and seeds (small portions)
Lifestyle Modifications
Stay Hydrated
Drink plenty of water throughout the day—aim for more than 2-3 liters daily. However, avoid drinking large amounts of liquid with meals, as this can increase stomach volume and pressure. Instead, sip water between meals.
Wear Loose-Fitting Clothing
Tight belts, waistbands, and clothing can put pressure on your stomach and worsen reflux. Choose comfortable, loose-fitting clothes, especially around your midsection.
Maintain a Healthy Weight
While you’re likely already working on weight loss with your GLP-1 medication, know that losing excess weight is one of the best long-term solutions for reducing reflux symptoms.
Avoid Smoking
Smoking weakens the valve between your stomach and esophagus and increases stomach acid production. If you smoke, talk to your healthcare provider about quitting strategies.
Limit Alcohol
Alcohol can worsen both nausea and reflux while on GLP-1 therapy. It’s best to minimize or avoid it, especially during dose adjustments.
Manage Stress
Stress can worsen digestive symptoms. Consider relaxation techniques like deep breathing, meditation, or gentle yoga.
When Symptoms Are Most Common
Heartburn and reflux symptoms are typically more noticeable:
- When you first start your GLP-1 medication
- After dose increases
- In the first few hours after taking your medication
- After eating large or fatty meals
- When lying down or bending over
Understanding these patterns can help you plan ahead and take preventive measures.
Over-the-Counter Relief Options
If lifestyle changes aren’t enough, several over-the-counter medications can help:
Antacids
Products like Tums, Rolaids, or Maalox provide quick, short-term relief by neutralizing stomach acid. They work within minutes but only last 1-2 hours.
H2 Blockers
Medications like famotidine (Pepcid) reduce acid production. They take longer to work than antacids (30-60 minutes) but last longer (up to 12 hours).
Proton Pump Inhibitors (PPIs)
Medications like omeprazole (Prilosec) or esomeprazole (Nexium) are the strongest acid reducers available over-the-counter. They work best when taken 30 minutes before your first meal of the day.
Important: Talk to your healthcare provider before starting any new medication, even over-the-counter options, to ensure they’re appropriate for your situation.
When to Contact Your Healthcare Provider
While heartburn is common with GLP-1 medications, certain symptoms require medical attention:
- Severe or persistent heartburn that doesn’t improve with lifestyle changes
- Difficulty or pain when swallowing
- Persistent nausea or vomiting
- Unintended weight loss
- Black, tarry stools or vomiting blood
- Chest pain (especially if it’s severe or accompanied by shortness of breath—call 911 if you’re unsure whether it’s heartburn or a heart problem)
- Symptoms that significantly interfere with your daily life or sleep
Your doctor may recommend prescription-strength medications or adjust your GLP-1 dose if symptoms are severe.
The Bottom Line
Many people successfully manage heartburn and reflux symptoms while continuing their GLP-1 therapy. The key is being proactive: eat smaller meals, avoid trigger foods, don’t lie down after eating, and stay well-hydrated. Most importantly, remember that these symptoms often improve as your body adjusts to the medication.
The benefits of GLP-1 therapy—better blood sugar control, weight loss, and reduced cardiovascular risk—are significant and long-lasting. With the right strategies, you can minimize discomfort and maximize the benefits of your treatment.
Work closely with your healthcare team to find the approach that works best for you. Don’t suffer in silence—there are many effective solutions available to help you feel comfortable while achieving your health goals.
By Dr. Efrain Santiago PharmD, MBA
Disclaimer
This information is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. The content provided should not replace professional medical advice from your healthcare provider. Always consult with your doctor, pharmacist, or other qualified healthcare professional before making any changes to your medication regimen, diet, or lifestyle, especially if you are taking GLP-1 medications or have any medical conditions. Individual responses to medications and dietary changes vary, and what works for one person may not be appropriate for another. If you experience severe or concerning symptoms while taking GLP-1 medications, contact your healthcare provider immediately or seek emergency medical care.
References
- Glucagon-Like Peptide-1 Receptor Agonists and Gastrointestinal Adverse Events: A Systematic Review and Meta-Analysis. Gastroenterology. 2025. Chiang CH, Jaroenlapnopparat A, Colak SC, et al.
- Glucagon-Like Peptide-1 Receptor Agonists and Risk for Gastroesophageal Reflux Disease in Patients With Type 2 Diabetes : A Population-Based Cohort Study. Annals of Internal Medicine. 2025. Noh Y, Yin H, Yu OHY, Bitton A, Azoulay L.
- Integrating Diet and Physical Activity When Prescribing GLP-1s—Lifestyle Factors Remain Crucial. JAMA Internal Medicine. 2025. Mehrtash F, Dushay J, Manson JE.
- Nutritional Priorities to Support GLP-1 Therapy for Obesity: A Joint Advisory From the American College of Lifestyle Medicine, the American Society for Nutrition, the Obesity Medicine Association, and the Obesity Society. The American Journal of Clinical Nutrition. 2025. Mozaffarian D, Agarwal M, Aggarwal M, et al.
- GLP1 and GIP Receptor Agonists: Effects on the Gastrointestinal Tract and Management Strategies for Primary Care Physicians. Mayo Clinic Proceedings. 2025. Saha B, Kamalumpundi V, Codipilly DC.
- Gastroesophageal Reflux Disease. The New England Journal of Medicine. 2022. Fass R.